Infection Risk with Epidural Anesthesia
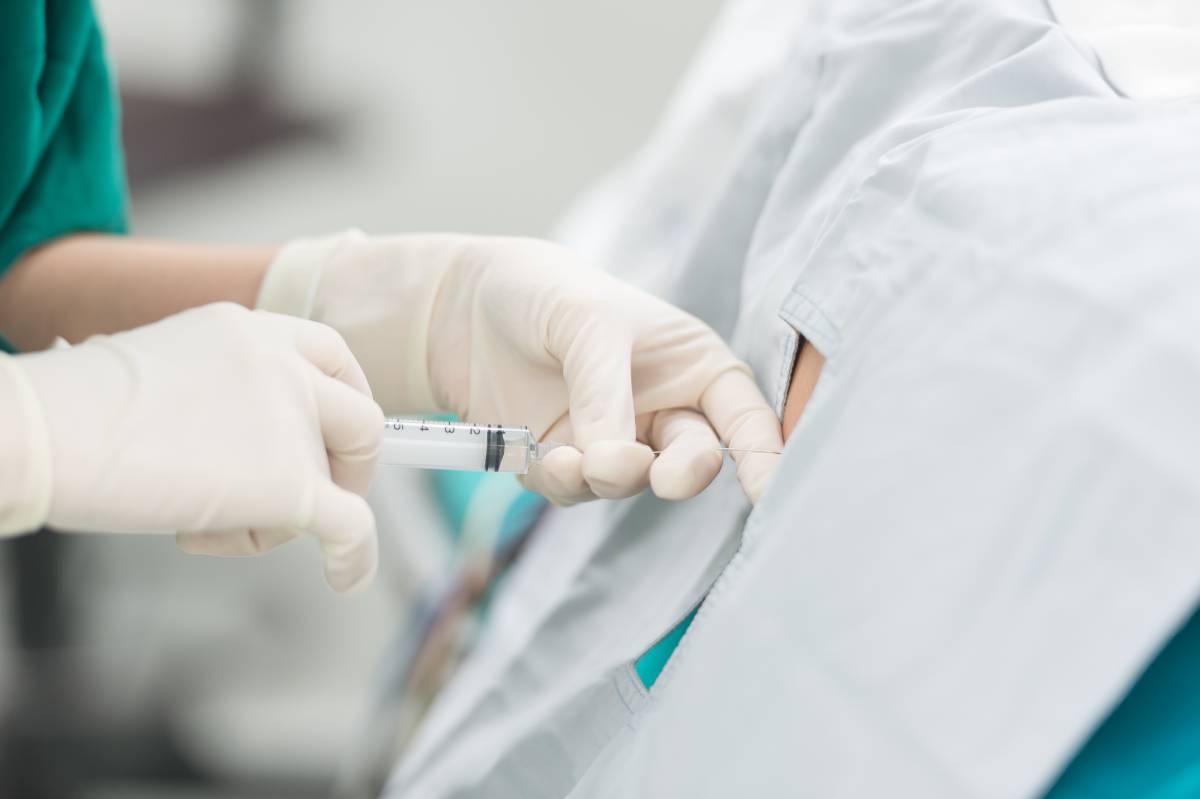
Epidural anesthesia is a useful and widespread technique to provide pain relief. It is safe and effective, but complications are still possible. A particularly problematic complication of epidural anesthesia is infection, which, in the epidural space, can become very serious 1. The infection risk linked to epidural anesthesia is low, but cases are likely to be underreported since most related information is only available in case reports and retrospective surveys 2.
A recent retrospective case note review sought to assess the types of complications linked to epidural anesthesia. Their analyses revealed six cases of epidural abscess, three of meningitis and three of epidural hematoma. Symptoms of meningitis tended to develop a median of 5 days after epidural catheter removal, and methicillin-resistant Staphylococcus aureus was the predominant pathogen causing infection after epidural anesthesia 3. Streptococcus pneumoniae, however, has also been shown to be a pathogen, and a number of additional case reports highlight associated complications including but not limited to meningitis, myelitis, tetraparesis, and paralysis 4.
Information on short-term infection risk linked to epidural anesthesia is available in certain clinical contexts. Rates associated with the short-term use of catheters in obstetrics, for example, have revealed that deep epidural infections affect 1 in 145,00 women 5. In obstetrics though, catheters are often in place for less than 24 hours. In cancer patients, however, they may be in place for months.
A recent study carried out a systematic review and pooled analysis of observational studies to assess infection rates with use of epidural catheters in place for seven days or more 6. Results demonstrated that approximately 1 in 35 patients with an epidural catheter in place for 74 days for relief of cancer pain may be expected to develop a deep epidural infection, and that approximately 1 in 500 may die of infection-related causes. However, these statistics need to be confirmed in different clinical scenarios to develop a more comprehensive understanding of infection risk for epidural anesthesia.
Children may also receive epidural anesthesia for procedures or for longer-term pain relief. A recent study from Children’s Hospital in Boston reviewed cases to assess whether suspected or confirmed epidural infection was associated with epidural analgesia among a large cohort of infants, children, and adolescents treated over a 6-year period 7. Overall, the researchers found that the risk of epidural infection to be quite low in pediatric postoperative patients receiving short-term catheterization for the administration of anesthesia. However, the use of prolonged epidural analgesia in the management of chronic pain in children still warrants careful monitoring for infection.
The clinical decision to implant an epidural catheter should be informed by the predicted benefits and risks of complications 6, knowing that robust estimates for the risk of infection have not yet been well-established.
Additional research is required in the near future in order to ensure the lowest infection risk possible with epidural anesthesia across clinical contexts. A detailed and comprehensive national database would allow for a more accurate estimate of the incidence of major complications and to pinpoint relevant risk factors 3. In the future, the integration of a structured surveillance tool into the electronic medical record and a hospital’s quality management system may facilitate reporting and research 2.
References
1. Nussbaum, E. S. et al. Spinal epidural abscess: a report of 40 cases and review. Surg. Neurol. 38, 225–231 (1992). DOI: 10.1016/0090-3019(92)90173-k
2. Infection Control in Regional Anesthesia – NYSORA | NYSORA. Available at: https://www.nysora.com/topics/complications/infection-control-regional-anesthesia/. (Accessed: 3rd June 2023)
3. Christie, I. W. & McCabe, S. Major complications of epidural analgesia after surgery: results of a six-year survey. Anaesthesia 62, 335–341 (2007). doi: 10.1111/j.1365-2044.2007.04992.x.
4. Bhattacharya, M. & Joshi, N. Spinal epidural abscess with myelitis and meningitis caused by Streptococcus pneumoniae in a young child. J. Spinal Cord Med. (2011). doi:10.1179/107902610×12883422813507
5. Ruppen, W., Derry, S., McQuay, H. & Moore, R. A. Incidence of epidural hematoma, infection, and neurologic injury in obstetric patients with epidural analgesia/anesthesia. Anesthesiology 105, 394–399 (2006). doi: 10.1097/00000542-200608000-00023.
6. Ruppen, W., Derry, S., McQuay, H. J. & Moore, R. A. Infection rates associated with epidural indwelling catheters for seven days or longer: systematic review and meta-analysis. BMC Palliat. Care 6, 3 (2007). doi: 10.1186/1472-684X-6-3.
7. The Risk of Infection from Epidural Analgesia in Children: A… : Anesthesia & Analgesia. Available at: https://journals.lww.com/anesthesia-analgesia/fulltext/1995/02000/the_risk_of_infection_from_epidural_analgesia_in.6.aspx. (Accessed: 3rd June 2023)
